Motor impairment includes impairments in the control of movement which incorporates the central nervous system, muscle function and motor performance https://motorimpairment.neura.edu.au/. Motor Impairment can therefore be seen as a pathway that causes physical disability in a wide range of these diseases (Figure 1). Our research has used falls as a paradigm to investigate to which extent various motor outputs, such as reaching, standing, stepping and walking, are dysfunctional. Within the motor impairment framework, falls can be viewed of what constitutes normal physiological performance.
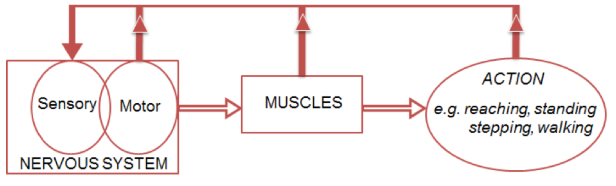
Figure 1. A conceptual model for the control of movement which emphasises that afferent feedback from muscles and motor actions arises continuously. This feedback needs to be processed with feedback from centrally generated motor signals. Deficits at any level are likely to impairments related to standing and locomotion.
The purpose of this article was to describe a physiological profiling approach for documenting motor impairments in older people at risk of falls and clinical groups with balance disorders. In essence, this approach involves the quantitative assessment of important physiological capacities required for stable mobility and fall avoidance, and the compilation of normative data that can be used as a reference for individual and disease group-based assessments. The article collated and summarised data from several studies that have used the Physiological Profile Assessment (PPA). It presented physiological profiles across a number of seemingly ‘single’ diseases or disability groups including people with multiple sclerosis, stroke, cognitive impairment, depressed mood, macular degeneration, lower limb osteoarthritis and prior polio. It emphasized that (i) motor impairment arises via reductions in a wide range of sensorimotor abilities; (ii) the PPA approach not only gives a snapshot of the physiological capacity of an individual, but also provides insight into the deficits among groups of individuals with particular diseases; and (iii) deficits in seemingly restricted and disparate physiological domains (e.g. vision, strength, cognition) are funnelled into balance and mobility impairments.
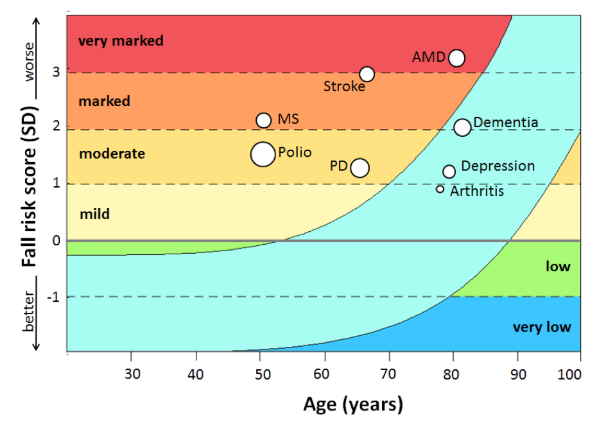
Figure 2. The overall PPA fall-risk scores is visualised for the clinical populations in relation to age, with the fall risk categorised from ‘very low’ to ‘very marked’. Ageing is associated with functional decline. The clinical groups all have high scores compared to their peers of the same age.
When used on an individual basis, the PPA can provide measurements of physiological frailty and fall risk, which can be used to guide subsequent personalised interventions to enhance mobility and reduce fall risk. Further, when viewed from the perspective of disease groups, this approach can provide insight into the physiology of tasks such as standing and walking and how these tasks are commonly affected in different diseases. With the challenges of population ageing, systematic approaches to motor impairment documentation and amelioration may assist older people and those with balance disorders to maintain functional abilities and independence.
Publication
Lord SR, Delbaere K, Gandevia SC. Use of a physiological profile to document motor impairment in ageing and in clinical groups. Journal of Physiology 2016;594:4513-4523. http://onlinelibrary.wiley.com/doi/10.1113/JP271108/pdf
About the Author

Stephen Lord
Professor and Senior Principal Research Fellow, Neuroscience Research Australia, University of New South Wales
Stephen Lord is a Senior Principal Research Scientist at Neuroscience Research Australia and chief investigator on NeuRA’s Motor Impairment Program https://motorimpairment.neura.edu.au/. He has published over 400 papers in the areas of balance, gait and falls in older people and is acknowledged as a leading international researcher in his field. His research follows two main themes: the identification of physiological risk factors for falls and the development and evaluation of fall prevention strategies.
Copyright
© 2018 by the author. Except as otherwise noted, the ISPGR blog, including its text and figures, is licensed under a Creative Commons Attribution-ShareAlike 4.0 International License. To view a copy of this license, visit https://creativecommons.org/licenses/by-sa/4.0/legalcode.
ISPGR blog (ISSN 2561-4703)
Are you interested in writing a blog post for the ISPGR website? If so, please email the ISGPR Secretariat with the following information:
- First and Last Name
- Institution/Affiliation
- Paper you will be referencing
