Difficulty turning, or changing direction of walking, is a major contributor to mobility disability, falls, and reduced quality of life in older people. The complex coupling of balance and locomotor systems -essential for turning- gradually deteriorates with ageing and neurological disorders. We speculated that turning speed might be more sensitive than gait speed to predict future falls, evaluate treatments, and indicate physical health. Currently, most studies on continuous monitoring of mobility focused on measuring activity, which reflects the quantity, but not the quality of mobility. Whilst informative, quantity measures may not characterize specific mobility impairments or capture qualitative patterns of daily activity. In this study, we compared the quantity and quality of turning in daily life, to discriminate between fallers and non-fallers.
Thirty-five elderly participants with a mean age of 88 years wore 3 Opal inertial sensors, one on their belt and on each foot, throughout 7 consecutive days in daily life. Quality of turning was assessed as the average and coefficient of variation of turn duration, turn rotational rate, and number of steps taken. In addition, quantity of mobility was assessed as the time spent walking and turning compared to total wear time, and as the number of turns per hour. Participants were grouped as non-fallers, single-fallers, and recurrent-fallers, based on their history of falls. We also followed patients for 6 months using weekly fall diaries to capture future falls.
We found that quality of turning was lower in recurrent-fallers compared to non-fallers and single-fallers. In contrast, quantity of mobility was similar across all groups. We further found that a higher day-to-day variability of the number of steps per turn was related to future falls (Figure 1). Our results indicate that the quality of turning, but not the quantity of turning, is compromised in people with a high risk of falls. Our results further indicate that day-to-day variation in turning quality might hold promise for identify individuals at risk for falls. This study is an essential step to overcome the critical barrier for neurologists and therapists to measure mobility in natural, functional settings since single event mobility measures in the clinic may not accurately reflect functional mobility. The assessment of quality of mobility during daily-life activities could serve as an approach to objectively quantify mobility function outside of the clinic, similarly to how a Holter monitor evaluates cardiac function over days and weeks. The developed method allows for evaluation of mobility across long periods of time to monitor risk for falls, fluctuations across the day, response to medication, etc.
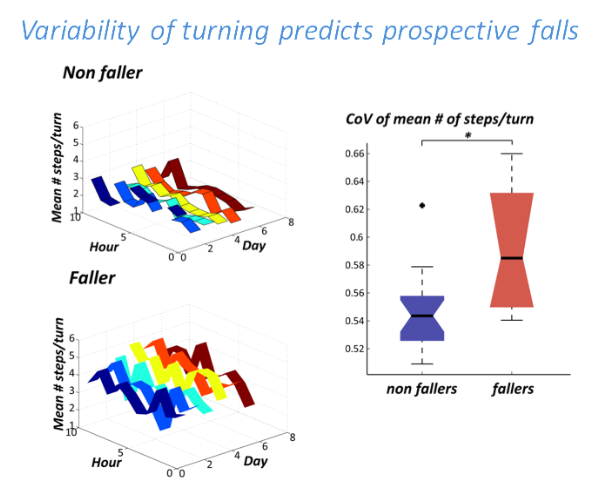
Figure 1: Left panel, Mean number of steps/hour per day in a representative future faller and non-faller. Right panel, Coefficient of Variation (CoV) of mean number of steps per turn across seven days in non-fallers and fallers.
Publication
Mancini, M., Schlueter, H., El-Gohary, M., Mattek, N., Duncan, C., Kaye, J., & Horak, F. B. (2016). Continuous monitoring of turning mobility and its association to falls and cognitive function: a pilot study. The Journals of Gerontology Series A: Biological Sciences and Medical Sciences.
http://biomedgerontology.oxfordjournals.org/content/early/2016/02/24/gerona.glw019.long
About the Author

Martina Mancini, PhD
Senior Research Associate Department of Neurology, Oregon Health & Science University
Martina Mancini, PhD, Senior Research Associate Department of Neurology, Oregon Health & Science University
Martina’s research focuses on understanding and characterizing the physiology and neural correlates of gait disturbances during locomotion with body worn sensors in subjects at risk for falls and neurological disease, and to determine whether biofeedback-based paradigms improve gait disturbances in a laboratory and home environment.
Copyright
© 2018 by the author. Except as otherwise noted, the ISPGR blog, including its text and figures, is licensed under a Creative Commons Attribution-ShareAlike 4.0 International License. To view a copy of this license, visit https://creativecommons.org/licenses/by-sa/4.0/legalcode.
ISPGR blog (ISSN 2561-4703)
Are you interested in writing a blog post for the ISPGR website? If so, please email the ISGPR Secretariat with the following information:
- First and Last Name
- Institution/Affiliation
- Paper you will be referencing
