Gait can tell us about our health, risk of falls and brain function. Gait problems are focal in Parkinson’s disease (PD): gait is slower with more asymmetry and variability than age-matched ‘controls’. Usually gait assessments are performed in laboratory settings with specialised equipment to accurately detect and quantify impairments. But does this paint a realistic picture of how people walk in their everyday life? During clinical assessments participants are more aware of their gait and may put on their best performance. So, we actually don’t know how people walk in their everyday life. We now have the technology to measure this. Body worn monitors (BWMs) can objectively measure walking behaviour over several days outside of the laboratory, in the real world. In this study we explore how a person’s daily environment and walking bout length can help better discriminating between PD and normal ageing gait.
Using a BWM placed on the lower back, we collected walking data of 47 PD participants and 50 healthy older ‘control’ participants both in laboratory and free-living (7 days) environments. Using validated methods we evaluated fourteen clinically relevant gait characteristics organised in five domains (pace, variability, rhythm, asymmetry, postural control). When analysing free-living gait, we used all walking bouts longer than 3 steps and looked at the effect of various bout length on gait. Most walking bouts were quite short and only 3% were longer than 60 seconds (s). In both groups, participants walked slower with higher variability, rhythm and asymmetry in free-living environments when compared to their gait test in the laboratory. When comparing healthy controls with PD participants, we saw that step length and velocity were different in both free-living and lab gait, while step length asymmetry and swing time were significantly different only in free-living conditions (Figure 1). Interestingly these differences depended on bout length and were more apparent during longer walking bouts. Bouts ≤10s did not discriminate between groups, while medium-to-long bouts highlighted differences for pace, rhythm and asymmetry.
This study provides encouraging results to support the use of BWMs for evaluating gait in free-living conditions. Findings from this study suggest that very short walking bouts do not discriminate between groups with a minimum of 10s required to detect changes in gait characteristics in PD. Measuring free-living gait is a challenge but holds great potential within clinical research. Our study showed that free-living measurements are more sensitive in discriminating pathology than laboratory-based data. Future work could investigate the medication effects on gait in PD and increase our understanding of gait in real-life environments – a potential red flag for underlying pathology!
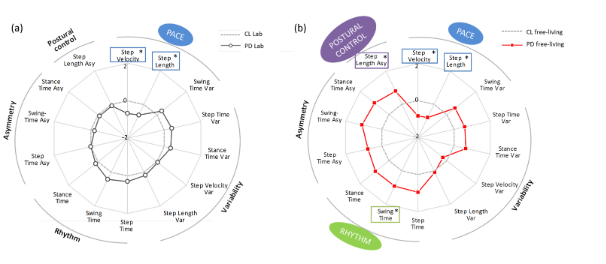
Figure 1: Radar plots illustrating the 14 gait characteristics organised by domain for people with Parkinson’s disease (PD) and controls (CL) evaluated in the lab (a) and in free-living conditions (b). The central dotted line represents CL data, deviation from zero along the axis radiating from the centre of the plot represents how many standard deviations (range: ± 2 SD, z score based on control means and standard deviations) the PD differ from CL. Asterisks represent significant differences between PD and CL.
Publication
Del Din S, Godfrey A, Galna B, Lord S, Rochester L. Free-living gait characteristics in ageing and Parkinson’s disease: impact of environment and ambulatory bout length. J Neuroeng Rehabil. 2016 May 12;13(1):46. doi: 10.1186/s12984-016-0154-5.
http://jneuroengrehab.biomedcentral.com/articles/10.1186/s12984-016-0154-5
About the Author
Silvia Del Din
Research Associate, Institute of Neuroscience (IoN)/Newcastle University Institute for Ageing, Newcastle University
I received my Bachelor’s Degree in Information Engineering in 2006 from the University of Padova (Italy) under the Supervision of Prof. Claudio Cobelli and my Master’s Degree (cum laude) in Bioengineering in 2008 from the University of Padova (“Biomechanical analysis of swimmers through markerless motion capture.” Supervisor: Ch.mo Prof. Claudio Cobelli, Co-advisor: Dr. Elena Ceseracciu).
In 2012 I completed my PhD in Bioengineering (Area of the Information Engineering PhD School) at the Department of Information Engineering of the University of Padova, under the supervision of Prof. Chiara Dalla Man (“Innovative Techniques for Biomechanical Evaluation of Stroke Survivors: Combined fMRI-Gait Analysis Assessment and Fugl-Meyer Clinical Scores Estimation Through Wearable Sensors.”).
From February 2012 until August 2012 I have been a Post Doctoral Fellow at the Department of Information Engineering of the University of Padova.
Since September 2012 I have been working as a Research Associate at the Institute of Neuroscience of Newcastle University in the Brain and Movement (BAM) Research Group led by Prof. Lynn Rochester.
Copyright
© 2018 by the author. Except as otherwise noted, the ISPGR blog, including its text and figures, is licensed under a Creative Commons Attribution-ShareAlike 4.0 International License. To view a copy of this license, visit https://creativecommons.org/licenses/by-sa/4.0/legalcode.
ISPGR blog (ISSN 2561-4703)
Are you interested in writing a blog post for the ISPGR website? If so, please email the ISGPR Secretariat with the following information:
- First and Last Name
- Institution/Affiliation
- Paper you will be referencing
